HbA1c vs daily blood sugar tests creates ongoing confusion among type 2 diabetes patients worldwide. Moreover, understanding both monitoring methods proves essential for optimal diabetes management and prevention of serious complications. Furthermore, each approach serves distinct purposes in comprehensive glucose control strategies.
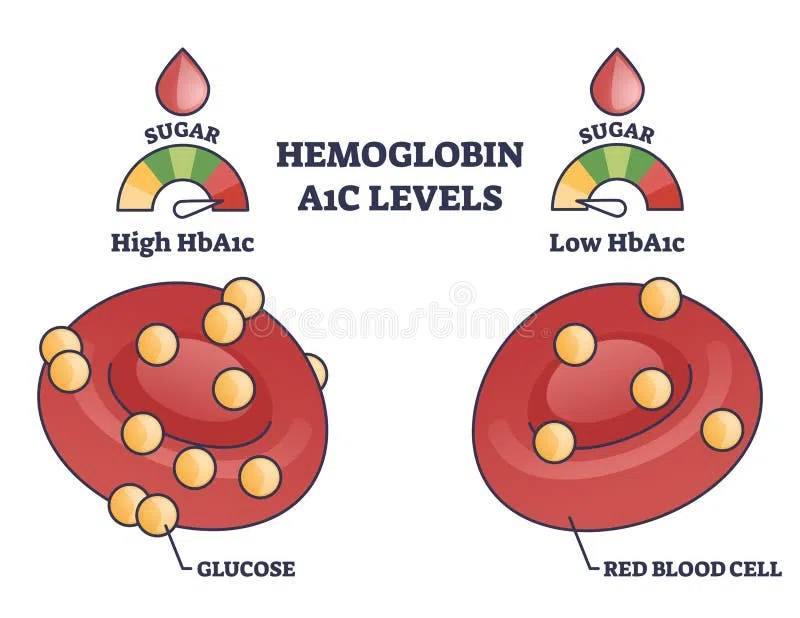
Diagram showing how glucose molecules attach to red blood cells, resulting in different Hemoglobin A1c levels indicating blood sugar control over time.
Understanding HbA1c: Your Long-Term Glucose Picture
HbA1c testing measures glucose attachment to hemoglobin over 2-3 months. Specifically, this test reveals average blood sugar levels during red blood cell lifespans. Additionally, healthcare providers use HbA1c results to assess treatment effectiveness and complication risks.
“Daily blood sugar checks show your sugar level at that moment, helping you understand how food, exercise, stress, or medicines affect you during the day,” explains Dr. Aarti Ullal
Normal HbA1c levels remain below 5.7% for non-diabetic individuals. Meanwhile, prediabetes ranges from 5.7% to 6.4%, while diabetes exceeds 6.5%. Consequently, patients should aim for individualized targets based on age and health conditions.
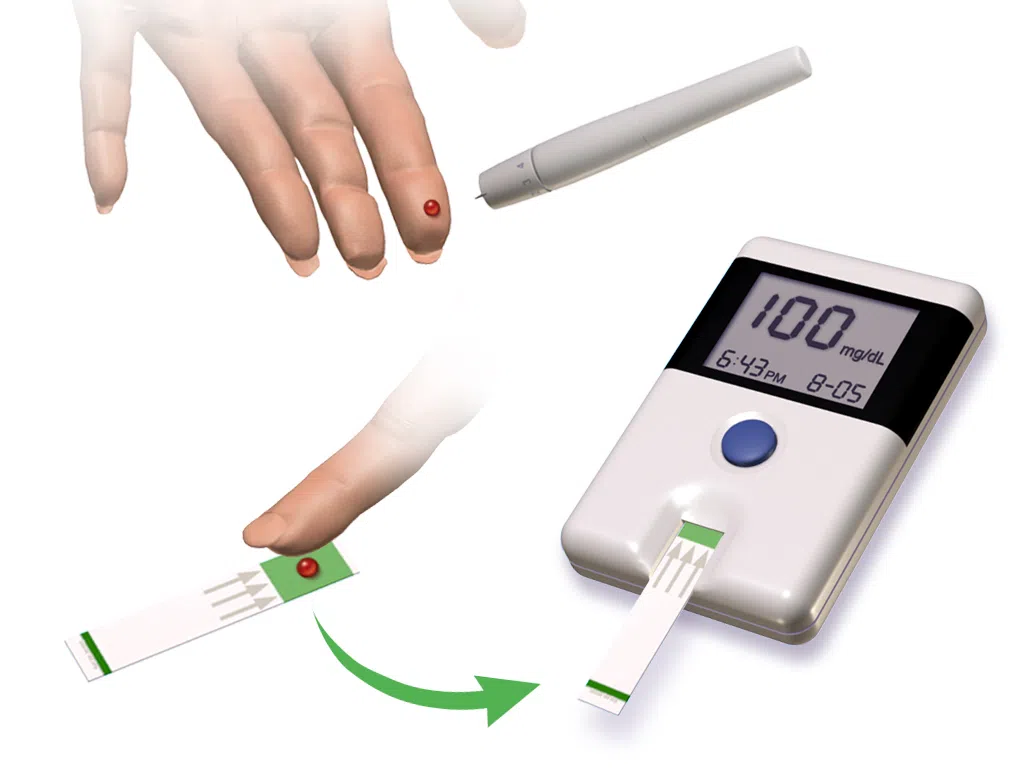
Fingerstick blood glucose testing with a digital glucose meter showing a blood sugar level of 100 mg/dL
Daily Blood Sugar Monitoring: Real-Time Glucose Insights
Daily glucose monitoring provides immediate blood sugar readings at specific moments. Thus, patients can make instant decisions about meals, exercise, and medication timing. Additionally, frequent testing helps identify dangerous highs and lows throughout the day.
Healthcare professionals recommend testing 2-4 times daily for insulin users. Meanwhile, non-insulin patients may test 2-3 times weekly or during illness. Furthermore, testing becomes crucial before meals, at bedtime, and during exercise.

Person performing fingerstick blood glucose test using a lancet device and glucose meter for daily diabetes monitoring.
Comparing HbA1c vs Daily Blood Sugar Tests Effectively
Both monitoring methods complement each other rather than compete for importance. Specifically, HbA1c reveals long-term patterns while daily tests show immediate variations. Therefore, combining both approaches creates comprehensive diabetes management strategies.
“Daily checks help with day-to-day management, while HbA1c helps track overall control and future risk of complications,” states Dr. Ullal.
However, HbA1c cannot detect daily glucose spikes or sudden drops. Conversely, daily testing misses long-term trends and treatment effectiveness patterns. Consequently, patients need both monitoring approaches for optimal diabetes control.
When Each Test Proves Most Valuable
HbA1c testing works best for quarterly treatment assessments and complication prevention. Moreover, doctors use these results to adjust medications and evaluate care plan success. Additionally, HbA1c helps predict cardiovascular and kidney disease risks effectively.
Daily monitoring becomes essential during medication changes, illness, or stress periods. Furthermore, patients benefit from frequent testing when adjusting insulin doses or meal plans. Similarly, exercise routines require careful glucose monitoring before and after activities.
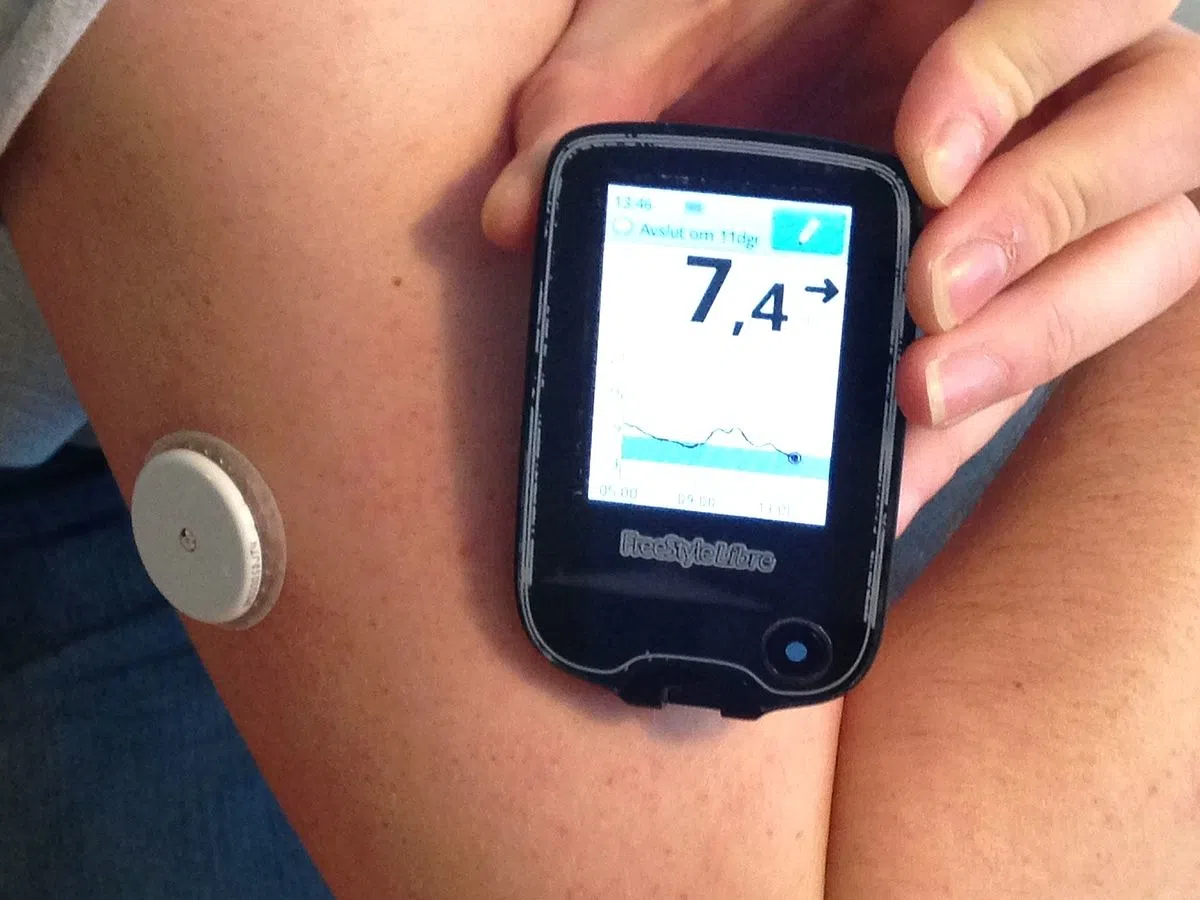
Continuous glucose monitoring sensor on arm with FreeStyle Libre reader showing blood glucose level and trends
Advanced Monitoring: Continuous Glucose Systems
Continuous glucose monitors (CGMs) bridge gaps between HbA1c and daily testing methods. Notably, CGMs provide real-time glucose readings every few minutes throughout the day. Moreover, these devices offer trend arrows showing glucose direction and rate changes.
Recent studies demonstrate CGM effectiveness across various diabetes treatment approaches. Specifically, patients using CGMs show significant HbA1c improvements compared to traditional testing. Additionally, CGMs detect nocturnal hypoglycemia episodes that fingerstick testing often misses.
“Continuous glucose monitoring devices are available, which help to measure real-time glucose, and they certainly help with dose adjustments,” notes Dr. Vyankatesh Shivane
Frequency Guidelines for Optimal Monitoring
Type 1 diabetes patients should test 5-8 times daily with traditional methods. Meanwhile, type 2 patients on insulin require 4+ daily tests during unstable periods. Furthermore, stable patients may reduce testing frequency to alternate days or weekly.
HbA1c testing occurs every 3-6 months depending on glucose control stability. However, poorly controlled patients may need quarterly testing until targets are achieved. Similarly, medication adjustments often require more frequent HbA1c monitoring.
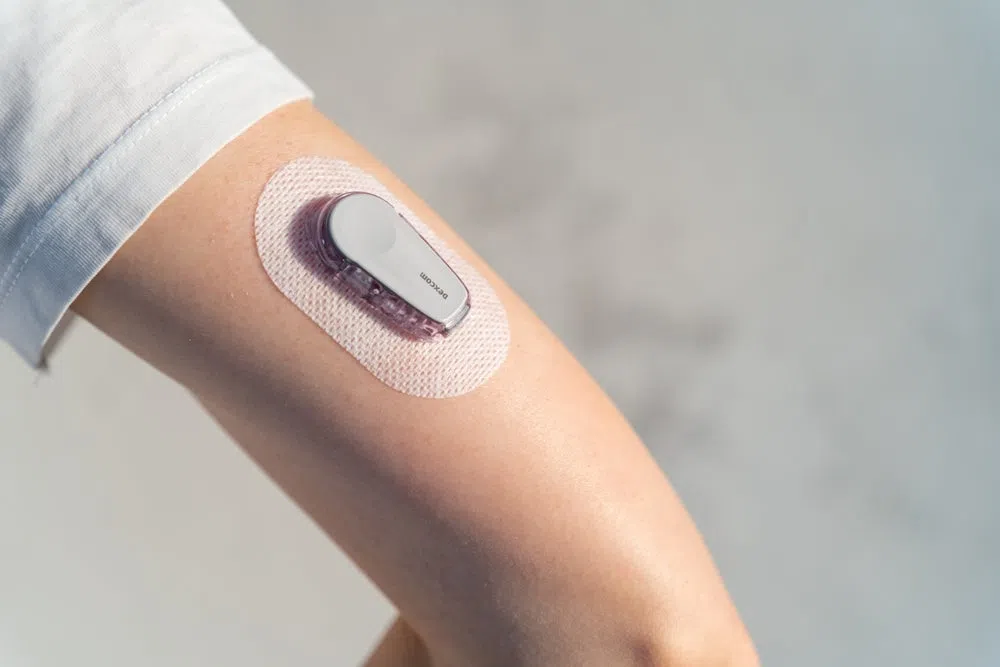
Continuous glucose monitor attached to a person’s arm for real-time blood sugar monitoring
Limitations and Special Considerations
HbA1c accuracy decreases in patients with certain blood disorders or kidney disease. Therefore, alternative tests like fructosamine may provide better glucose assessment. Additionally, pregnancy, recent blood loss, or iron deficiency can affect HbA1c reliability.
Daily testing faces challenges including finger pain, cost, and compliance issues. Moreover, patients may skip testing during busy schedules or stressful situations. Furthermore, meter accuracy varies between brands and requires proper calibration.
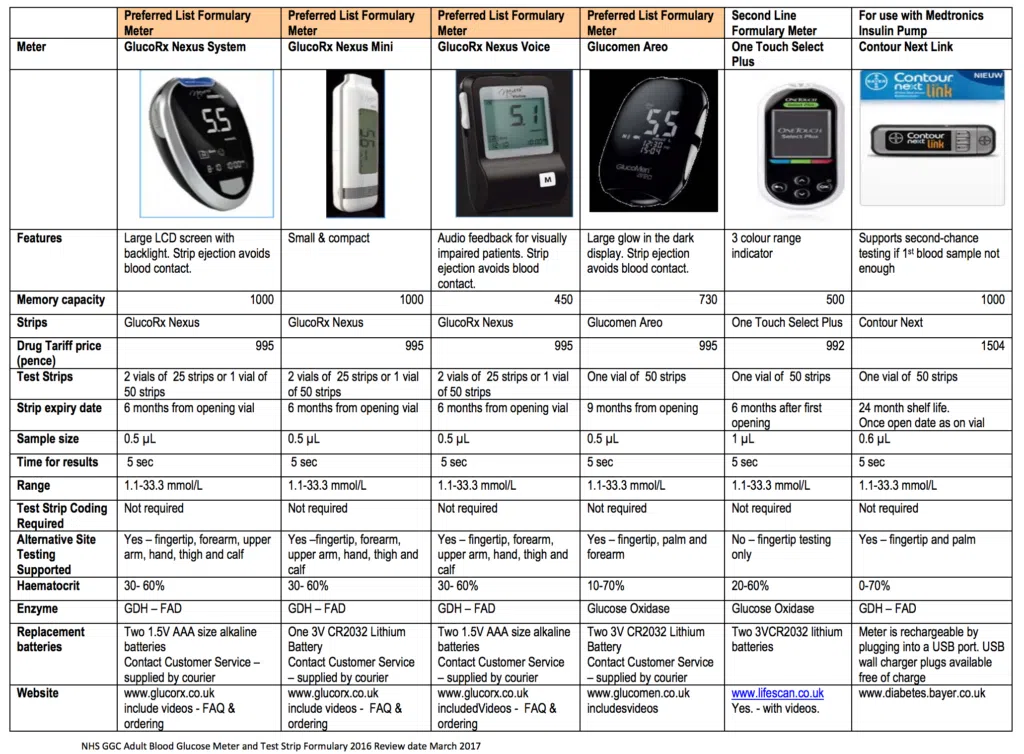
Comparison chart of different blood glucose meters outlining features, testing requirements, and device specifications relevant for diabetes management
Cost-Effectiveness and Practical Benefits
CGM systems demonstrate long-term cost-effectiveness despite higher upfront expenses. Specifically, reduced hospitalizations and complications offset device costs over time. Additionally, improved quality of life and reduced hypoglycemia fear provide significant patient benefits.
Traditional daily testing remains affordable but requires ongoing strip purchases. Meanwhile, HbA1c testing costs less per test but provides limited actionable information. Consequently, insurance coverage often favors comprehensive monitoring approaches combining multiple methods.
Making Informed Monitoring Decisions
Healthcare providers should individualize monitoring strategies based on patient needs and resources. Moreover, treatment complexity, hypoglycemia risk, and lifestyle factors influence optimal testing frequency. Additionally, patient education about interpreting results improves diabetes self-management success.
Technology integration helps patients track patterns and share data with providers effectively. Furthermore, smartphone apps simplify record-keeping and trend analysis for better decision-making. Therefore, modern diabetes management combines traditional testing with innovative monitoring solutions.
Both HbA1c vs daily blood sugar tests serve crucial roles in comprehensive diabetes care strategies. Ultimately, combining these monitoring approaches provides the most complete picture of glucose control and helps prevent serious complications while improving quality of life for diabetes patients.
DISCLAIMER: This article is based on information from the public domain and/or the experts we spoke to. Always consult your health practitioner before starting any routine.






